La Chirurgia Cosmetica Morfodinamica e le sue tecniche si basano su concetti interdisciplinari provenienti dall’Anatomia Funzionale, Ortopedia e Crescita Cranio-Facciale, Meccanobiologia, Craniologia Funzionale, Proloterapia, su recenti acquisizione riguardo i complessi network neuromuscolari dei tessuti, su recenti ricerche riguardanti i biomateriali, la medicina rigenerativa e bioingegneria.
Il principio fondamentale della Chirurgia Cosmetica Morfodinamica è che: la funzione determina la forma. Ossia la morfologia del nostro viso (e ovviamente di tutto il corpo) è solo in parte dovuta a fattori genetici, le dinamiche dei complessi network neuromuscolari ne determinano lo sviluppo e l’evoluzione, per cui modificando queste dinamiche si ottengono notevoli cambiamenti (principio della matrice funzionale di Moss).
Il network neuro-muscolare mediante la stimolazione della matrice periostale causa la crescita diretta dell’unità microscheletrica (comprendente ossa, cartilagini e tessuti tendinei), il meccanismo di deposizione ossea e riassorbimento sotto carico porta ad effetti sulla misura e/o forma della struttura ossea. Come per i muscoli, infatti, che tendono a ingrossarsi e irrobustirsi col tempo a seguito di adeguati stimoli o ad atrofizzarsi in mancanza di tali, anche per le ossa il nostro corpo applica questo tipo di meccanismo.
È su queste concetti che si basano il metodo e le tecniche della Chirurgia Cosmetica Morfodinamica per ottenere rimodellamento dei tessuti, compresi muscoli ed ossa. Un altro principio fondamentale della Chirurgia Cosmetica Morfodinamica è la esclusione di incisioni chirurgiche lineari (come quelle della blefaroplastica e dei lifting), ove possibile. Questo perché le cicatrici lineari che residuano interrompono le fisiologiche dinamiche dei network neuromuscolari dando negli anni successivi esiti sgradevoli. Per ovviare a questo si dà grande rilievo a tecniche mini invasive come quelle dei fili.
Nel mondo dell’estetica gran parte delle procedure cercano di ottenere una blanda fibrosi per rassodare i tessuti cutanei e sottocutanei aumentando l’attività dei fibroblasti, ossia di quelle cellule deputate alla produzione di matrice connettivale. Quindi qualsivoglia filler (acido ialuronico, polilattico, policaprolattone, idrossiapatite, etc.), filo biostimolante o di trazione, radiofrequenza, ultrasuoni focalizzati e non, ozonoterapia, vari tipi di laser, biostimolazioni, etc. in misura maggiore o minore, hanno la finalità di stimolare la produzione endogena di collagene per ottenere dei tessuti più sodi ed un aspetto più giovanile.
In Chirurgia Cosmetica Morfodinamica vengono utilizzati fili di diversa composizione, a rapido (PDO, PLA) e lento riassorbimento (poliammide).
Secondo la United States Farmacopea le suture sono considerate riassorbibili quando sono dissolte in vivo entro sei mesi, oltre questo periodo sono considerate permanenti o non riassorbibili.
Tuttavia studi specialistici sul comportamento in vivo dei polimeri e biomateriali evidenziano che tra le suture non riassorbibili (poliammide, polietilene, poliestere, polivinildenefluoride, seta, …) la poliammide, grazie alla sua struttura polipeptidica e ai gruppi ammidici (ha una struttura chimica simile al collagene), e alla sua capacità di incorporare acqua fino al 10% della sua massa, è il materiale che subisce maggiormente il naturale processo di idrolisi in vivo (circa il 20-25% ad anno), per questi motivi la poliammide è il materiale più utilizzato in Chirurgia Cosmetica Morfodinamica.
La poliammide multifilamenti, non rivestita (quindi senza silicone, cera o altro) subisce il processo di idrolisi molto più intensamente rispetto alle suture monofilamento e alle suture multifilamenti rivestite. La struttura multifilamenti è composta da una miriade di filamenti sottilissimi intrecciati tra di loro, questa struttura insieme all’assenza di qualsiasi rivestimento favoriscono l’azione enzimatica (il polietilene è il più resistente, tra i polimeri il polimetilmetacrilato rimane intatto all’attività degli enzimi) (Karaka E. et al).
Infatti il formato monofilamento della poliammide viene adoperato quando si vuole ridurre al minimo le possibilità di riassorbimento, mantiene le proprie caratteristiche morfologiche e fisiche per molto più tempo, è indicato in cardiochirugia, gastroenterologia, oculistica, neurochirurgia, ortopedia, protesi capelli, etc. Il formato multifilamenti è più adatto per legature vasi, fascia, peritoneo, chirurgia plastica, chirurgia generale, quale medicazione di ferite croniche, etc. Per la sua alta biocompatibilità, capacità biomimetica e alta biodegradabilità, la poliammide viene applicato come veicolante di farmaci e supporto di tecniche rigenerative.
Il Prof. Karaka, Department of Textile Engineering, Faculty of Engineering and Architecture, Uludag University, in una delle sue pubblicazioni scrive” Among the synthetic nonabsorbable sutures, polyamides are probably the one most susceptible to degradation in vivo”.
Lo stesso tipo di materiale viene adoperato dal Prof. Nikolay Serdev, autore di numerose pubblicazioni su tecniche mini invasive. Le sue suture in polycaproamide vengono descritte nel libro del dott. Bacci “semipermanenti e semielastiche, a lento riassorbimento, dai 3 ai 5 anni” (Bacci, La bellezza appesa ad un filo. Minelli Editore. Pag 49).
Le Sedev Suture Polycon sono realizzate in poliammide (polycaproamide) bulgaro con aggiunta di un antimicrobico, sono semielastiche ed assorbibili a lungo termine (2-3 anni), sul sito Medical Devices Int. si legge: “Long-term Absorbable – the surgical threads are absorbed in the human body within two years” ( https://medicaldevices-bg.com/surgical-sutures/). La policaproammide è uno specifico tipo di poliammide (nylon 6).
La poliamide 6 (PA6, Nylon6, da cycloexanone via e-caprolactam) e la poliammide 6,6 (PA66, Nylon6,6, da adipic acid e hexamethylene ), specialmente nella forma intrecciata e non rivestita, possono essere considerate “materiale a lento riassorbimento”, grazie alla loro idrofilia e suscettibilità alla degradazione idrolitica in vivo. La poliammide 6 assorbe circa il 9-10% di acqua, la poliammide 6,6 il 4-5% di acqua. Entrambi questi materiali vengono utilizzati in vivo come impianti semidegradabili. La poliammide 6 si degrada in vivo più velocemente della poliammide 6,6 per idrolisi dei legami ammidici, un processo accelerato in ambienti fisiologici umidi e con enzimi specifici. Inoltre la PA6 ha una minore cristallinità (~40%) rispetto alla PA66 (~50-55%). Una minore cristallinità significa che la PA6 ha più regione amorfe, dove l’acqua può penetrare più facilmente e accelerare la degradazione idrolitica, questa è particolarmente presente in ambienti fisiologici con pH vicino alla neutralità o leggermente acido (come nei tessuti infiammati). Per tutti questi motivi la PA6 viene preferita alla PA66 per dispositivi medici impiantabili bioassorbibili proprio grazie alla sua biodegradabilità quando si vuole un più rapido riassorbimento e per questi motivi le suture in poliammide 6 vengono definite a “lento riassorbimento “, pur appartenendo alla categoria delle suture non riassorbibili.
Una delle complicanze più frequenti nella metodica di inserimento di fili chirurgici a lento riassorbimento è l’eccessiva fibrosi.
In caso di fibrosi in eccesso vanno effettuate infiltrazioni intralesionali di sostanze o farmaci con azione fibrinolitica o stimolante la rigenerazione dei tessuti.
Le sostanza e farmaci utilizzati sono: kenacort, ialuronidasi, collagenasi (PB Serum), 5-fluorouracile, eparina, pentossifillina, verteporfina, verapamil, imiquimod 5%, acido ialuronico, tossina botilinica, etc. È possibile utilizzare tecniche rigenerative con fattori di crescita (PRP naturali o biomimetici) con cellule staminali prelevate dal grasso autologo: (microfat e nanofat), etc.
Dopo diversi mesi nelle fibrosi possono precipitare sali minerali creando delle calcificazioni, in tal caso si adopera:
▪ il tiosolfato sodico, molto efficace in tutte le lesioni da deposito di calcio (calcinosi),
▪ la pentossifillina, che aumenta la microcircolazione nei tessuti con placche calcificate e fibrotiche, riduce il deposito di collagene I e riduce la calcificazione.
La seconda possibilità terapeutica è la terapia sistemica con svariate sostanze, tra cui prednisolone, minociclina, allopurinolo, colchicine, ciclosporine, methotrexate, sostanze fibrinolitiche (serrapeptasi, etc) etc. Buoni risultati sono stati ottenuti anche con la terapia fotodinamica.
Come ultima possibilità c’è la chirurgia, ma solo se tutte le altre non hanno avuto successo. La chirurgia mai è la prima scelta, tranne in caso dei granulomi piogenici (di ben altra natura ed istologia). Eseguire chirurgia per rimuovere tessuto fibrotico senza aver prima tentato le metodiche conservative espone a maggiori rischi il paziente sia per le cicatrici residue che per i rischi insiti nella procedura chirurgica.
Bibliografia:
- Abdal-hay A., et al.: Biocompatibility property of polyamide 6/PCL blends composite textile scaffold usingEA.hy926 human endothelial cells. Biomed Mater. 12 (2017)1-12
- Abdallah Gomaa A, Comparison between intralesional injection of botulin toxin A and triamcinolone in management of recent hypertrophic scars. Zagazig Un Med J.vol 30, issue 1.1-january 2024
- Abdel Fattah AAE, Intralesional injection of hyaluronic acid compared with verapamil in acute phase of Peyronie’s disease: A prospective randomized clinical trial. Arab J Urol. 2024 Mar 22;22(4):206-211
- AbrahamR. F.De FattaR. J.Williams III E.F.: “Thread-lift for facial rejuvenation. Assessment of long-term results”Arch. Facial Plast. Surg. 1131781832009
- Adil A, Comparison of efficacy and safety of intralesional verapamil hydrocloride and intralesional triamcinolone in tha treatment of keloids. J of Pakistan Ass of Dermat.Vol 34 n1 (2024):january-march
- Ahn K and H. J. Choi, “Complication After PDO Threads Lift,” Journal of Craniofacial Surgery 30 (2019): e467–e469.
- Almadori A. Scarring and Skin Fibrosis Reversal with Regenerative Surgery and Stem Cell Therapy 2024 3;13(5):443
- Anderson JM, alia – Foreign body reactions to biomaterials. Semin Immunology, 2008
- Anderson J. Biocompatibility and bioresponse to biomaterials. Principles of Regenerative Medicine. 2008 –
- Anderson J. Perspective on the inflammmatory healing and foreign body responses to biomaterials and medical devices. Host Response to Biomaterials. 2015
- Antonio CR. Cells biomodulation: the future of Dermatology. Surg Cosmet Dermatol. Rio de Janeiro v.11 n.1 jan-mar. 2019 p. 11-8.
- Argentati C., et alium. Insight into Mechanobiology: How Stem Cells Feel Mechanical Forces and Orchestrate Biological Functions. Int J Mol Sci. 2019 Oct 26;20(21):5337.
- Armentano I., Gigli M., Morena F., Argentati C., Torre L., Martino S. Recent advances in nanocomposites based on aliphatic polyesters: Design, synthesis, and applications in regenerative medicine. Appl. Sci. 2018;8:1452.
- Auriemma M., et al.: Treatment of calciphylaxis with sodium thiosulfate: two cases report and review of the litterature. Am Lornal of Dermatology. 2011,12(5),339-46
- Bacci P. A.: Chirurgia estetica mini invasiva con fili di sostegno. Minelli Editore 2006
- Bacci P. A. : Fill traction in PDO. La bellezza appesa a un filo. Mini lift e trattamenti dermocosmetici. Editore OEO, 2020
- Bacci P.A.: T3 – Soft Face Lift by Suspension Surgery. Published: 02 October 2013, Intech Open.
- Behrents RG. Growth in the Aging Craniofacial Skeleton. Craniofacial Growth Series. Ann Arbor, MI: Center for Human Growth and Development, University of Michigan; 1985. Monograph #17.
- Blugerman G., et al.: Five fluorouracil, hyaluronidase, and triamcinolone in the nasal region. Mininvasive techniques in rhinoplasty. Cap 11. 2016
- Bolamperti S., et al.: Bone remodeling: an operational process ensuring survival and bone mechanical competence. Bone Research. July 2022 , 10(1):48
- Borovikova AA, Adipose-Derived Tissue in the Treatment of Dermal Fibrosis: Antifibrotic Effects of Adipose-Derived Stem Cells. Ann Plast Surg. 2018 Mar;80(3):297-307.
- Broly M., alia – Management of granulomatous foreign body reaction to fillers with methotrexate JEADV 2019
- Bush JO, Jiang R. Palatogenesis: morphological and molecular mechanisms of secondary palate development. Devel. 2012;139:231–243.
- Buschang PH, Hinton RJ. A gradient of potential for modifying craniofacial growth. In: Carlson DS, ed. Control Mechanisms of Craniofacial Development and Growth. Semin Orthod; 2005; 11(4):219226.
- Buschang PH, Jacob HB, Demirjian A. Female adolescent craniofacial growth spurts: real or fiction? Eur J Orthod. 2013;35:819–825.
- Capurro S.: “The double tipped needle”Plast. Reconst. Surg., June 1987
- Capurro Sergio. Canale YouTube riguardante le tecniche del Prof. Sergio Capurro con fili elastici: https://www.crpub.org/
- Capurro Sergio. Link della bibliografia riguardante le tecniche del Prof. Sergio Capurro con fili elastici: https://www.crpub.org/publications
- Carlson DS. Theories of craniofacial growth in the postgenomic era. In: Carlson DS, ed. Control Mechanisms of Craniofacial Development and Growth. Semin Orthod; 2005;11(4):172–183.
- Carnicer-Lombarte A.:Foreign body reaction to implanted biomaterials . Front Bioeng Biotechnol, 15 april 2021. Vol9-2021
- Carlson DS. Growth modification: from molecules to mandibles. In: McNamara JA, ed. Growth Modification: What Works, What Doesn’t, and Why. Craniofacial Growth Series. Ann Arbor, MI: Center for Human Growth and Development; 1999:17–65.
- Cavanzo N. P., et al.: Verteporfin ameliorates fibrotic aspects of Dupuytren’s disease nodular fibroblasts irrespective the activation state of the cells. Scientific Reports.13940. 2022
- Cervelli V, Gentile P, De Angelis B, et al. Application of enhanced stromal vascular fraction and fat grafting mixed with PRP in post-traumatic lower extremity ulcers. Stem Cell Res. 2011;6 (2):103–111.
- Chalouhi M. Treatment of facial subcutaneous fibrosis with hyaluronic acid. The PMFA Journal, oct-nov 2021, vol 9,n 1.
- Chellamani K.P. et al.: Surgical sutures: an overview. J Acad. Indust. Vol 1(12) may 2013
- Chai Y, Maxson Jr RE. Recent advances in craniofacial morphogenesis. Dev Dyn. 2006;235
- Chang, C.; Medical Fibers and Biotextiles. In Biomaterials Science; Academic Press: Cambridge, MA, USA, 2020; pp. 575–600.
- Cheong EC, Leow YH. Extrusion of suture and granuloma formation from a neck thread lift. Dermatol Online J. 2021;27(9). 30.
- Chia-Hsiang Y. Ph driven continous stem production with enhanced regenerative capacity from polyamide/chitosan surfaces. Materials today bio. 18 (2023) : “Polyamide-66 (PA) is a synthetic polymer that bears a resemblance to collagen in its backbone and has excellent stability and biocompatibility [Winnaker].
- Choi EJ, Intralesional Injection Therapy and Atypical Peyronie’s Disease: A Systematic Review. Sex Med Rev. 2021 Jul;9(3):434-444
- Cilio S. Intraplaque injections of hyaluronic acid for the treatment of stable-phase Peyronie’s disease: a retrospective single-center experience. Working Group Sexual and Reproductive Health.Asian J Androl. 2024 May 1;26(3):268-271.
- ConstantinidesM. S.GalliS. K.MillerP. J.AdamsonP. A.Malar, submalar, and midfacial implants. Facial Plast Surg 20001613544
- Coury A.: Chemical and biochemical degradation of polymers intended to be biostable. Biomaterials Science (Fourth Edition) 2020, pages 919-940.
- Del Burgo L. 3D printed porous polyamide macrocapsule combined with alginate for safer cell-based therapies. Scientific Reports 31may 2018
- Des Fernandes. Suspension Sutures to Change the Nasal Tip. Submitted: 29 April 2012 Published: 02 October 2013 Intech Open
- Dullea A, In vitro efficacy of intralesional Collagenase Clostridium Histolyticum for the treatment of calcified Peyronie’s disease plaques. J Impot Res. 2024 Sep;36(6):572-575.
- EremiaS.WilloughbyM. A.Novel face-lift suspension suture and inserting instrument: use of large anchors knotted into the suture with attached needle and inserting device allowing for single entry point placement of suspension suture. Preliminary report of 20 cases with 6- to 12-month follow-up”. Dermatol. Surg. 32335452006
- Eriksen EF, LangdahlB.1995. Bone remodeling and its consequences for bone structure. In Bone Structure and Remodeling, ed. A Odgaard, H Weinans, pp. 25–36. London: World Sci.
- Feng F.: Biomechanical regulatory factors and terapeutic targets in keloid fibrosis. Frontiers in Pharmacology. May 2022
- Fronza M., Caetano G., alia – Hyaluronidase Modulates Inflammatory Response and Accelerates the Cutaneous Wound Healing. – PLOSE ONE – November 2014, Issue 11
- Frost HM : Bone Remodelling Dynamics. Springfield, IL: 1986.Intermediary Organization of the Skeleton. BocaRaton,FL:CRC Press Frost HM. 1973.
- Gentile P, Scioli MG, Bielli A, et al. Comparing different nanofat procedures on scars: role of the stromal vascular fraction and its clinical implications. Reg Med. 2017;12(8):939–995.
- Gentile P. Regenerative Plastic Surgery. Nova Medicine and Health. 2021
- Gentile P, Calabrese C, De Angelis B, et al. Impact of the different preparation methods to obtain human adipose-derived stromal vascular fraction cells (AD-SVFs) and human adipose-derived mesenchymal stem cells (AD-MSCs): enzymatic digestion versus mechanical centrifugation. Int J Mol Sci. 2019;20(21):5471.
- Gentile P, Garcovich S. Systematic Review: Adipose-derived mesenchymal stem cells, platelet-rich plasma and biomaterials as new regenerative strategies in Chronic Skin Wounds and soft tissue defects. Int J Mol Sci. 2021;22(4):1538.
- Gentile P, Sterodimas A, Pizzicannella J, et al. Systematic review: allogenic use of stromal vascular fraction (SVF) and decellularized extracellular matrices (ECM) as advanced therapy medicinal products (ATMP) in tissue regeneration. Int J Mol Sci. 2020;21 (14):1–14.
- Gentile P, Bottini DJ, Spallone D, et al. Application of platelet-rich plasma in maxillofacial surgery: clinical evaluation. J Craniofacial Surg. 2010;2(3):900–904.
- Gentile P, Cole JP, Cole MA, et al. Evaluation of not-activated and activated PRP in hair loss treatment: role of growth factor and cytokine concentrations obtained by different collection systems. Int J Mol Sci. 2017;18:408.
- Gentile P. Autologous cellular method using micrografts of human Adipose Tissue derived Follicle Stem Cells in Androgenic Alopecia. Int J Mol Sci. 2019;13:20.
- Göpferich A. Mechanism of polymer degradation and erosion. Biomaterials, 31(1996)Jan;17(2): 103-14.
- Graziosi A., C.Beer SMC.: Brow lifting with thread: the technique without undermining using minimum incisions. Aesthetic Plast Surg 1998Mar-Apr;2221205
- GrossE. J.HamiltonM. M.AckermannK.PerkinsS. W.Mersilene mesh chin augmentation. A 14-year experience.Arch Facial Plast Surg 1999Jul-Sep;131839
- Hayden M.R., et al.: Sodium thiosulfate: new hope for the treatment of calciphylaxis. Semin Dial. 2010;23(3) 258-2636
- HellingE. R.OkpakuA.WangP. T. H.LevineR. A.Complications of facial suspension suturesAesth. Surg J.271551612007
- Hillam RA, Skerry TM. 1995. Inhibition of bone resorption and stimulation of formation by mechanical loading of the modeling rat ulna in vivo. J. Bone Miner. Res. 10:683–89
- Ho Han J., Kim J., alia – Treatment of post traumatic hematoma and fibrosis using hyaluronidase injection. – ACFS – december 2017
- Hoffman T., Khademhosseini A., Langer R. Chasing the Paradigm: Clinical Translation of 25 Years of Tissue Engineering. Tissue Eng. Part A. 2019;25:679–687.
- Holan V. The growth and delivery of mesenchymal and limbal stem cells using copolymer polyamide6/12 nano fiber scaffolds. Methods Mol Biol 2013:1014:187-99
- Hong Y, et al.: The mechanobiology of fibroblast activation. Biophysical Journal 10 february 2023
- Hong and E. Park, “Granuloma Formation, a Rare Complication After PDO Threads Lifting, and Adjuvant Treatment Using Dual-Frequency Ultrasound (LDM® -MED),” Medical Lasers 8 (2019): 35–38.
- HorneD. F.KaminerM. S.Reduction of face and neck laxity with anchored, barbed polypropylene sutures (Contour Threads).Skin Therapy Lett. 111572006
- Huang J.: The long-term behavior and differences in bone reconstruction of three polymer-based scaffolds with different degradability. Journal of materials chemistry. B, 2019, 7,7690
- Huang D. et al.: Bioactive composite gradient coatings of nano-hydroxyapatite/polyamide 66 fabricated on polyamide66 substrates. J R. Soc. Interface, 2012, 9,1450-1457
- Hudson J. A., et al.: The in vivo biodegradation of nylon 6 utilized in a particular IUD. J Biomater. Appl. 1 (1987) 487-501.
- HudsonD. A.FernandesD. B.Caveats for the use of suspension sutures”Aesth. Plastic Surg. 281701732004
- Ingber D, et al.: Interdisciplinarity of mechanobiology. Science, 28 april 2022
- Jansen K.A., Donato D.M., Balcioglu H.E., Schmidt T., Danen E.H.J., Koenderink G.H. A guide to mechanobiology: Where biology and physics meet. Biochim. Biophys. Acta. 2015;1853:3043–3052.
- Jebors S. Turning peptides into bioactive nylons. European Polymer Journal 135 (2020)
- Jeong M. L., Yu J. K. – Successful treatment of foreign body granuloma using topical photodynamic therapy. Med Laser 2014
- Jeong M. L., Yu J. K. – Foreign body granulomas after the use of dermal fillers: pathophysiology, clinical appearance, histologic features and treatmemt. Korean Society of Plastic Surgery 2014
- Jeong M. L., Yu J. K. – Foreign body granulomas after the use of dermal fillers: pathophysiology, clinical appearance, histologic features and treatmemt. Korean Society of Plastic Surgery 2014
- Karaka E.: Analysis of the fracture morphology of polyamide, polyester, polipropylene, and silk stutures before and after implantation in vivo. Journal of biomedical material research. Part B: Applied Biomaterials
- Karaka E. et al.: Investigating changes in mechanical properties and tissue reaction of silk, polyester, polyamide and polypropilene sutures in vivo. Textile Research Journal. April 1, 2005
- Khadka A., et al.: Evaluation of hybrid porous biomimetic nano-hydroxyapatite/polyamide 6 and bone marrow-derived stem cell construct in repair of calvarian critical size defect. Journal of craniofacial surgery, 2011
- Khatery BH. Assessment of intralesional injection of botulinum toxin type A in hypertrophic scars and keloids: Clinical and pathological study. 2022;35(10):e15748.
- KheirJ. N. Polydimethylsiloxane for augmentation of the chin, malar, and nasal bones.J Long Term Eff Med Implants 1998815567
- Kyu-Ho Yi, Soo Yeon Park. Facial Thread Lifting Complications . Cosmetic Dermatology : 06 January 2025 https://doi.org/10.1111/jocd.16745
- Kuhn JL, Ciarelli MJ. The biomechanics of the growth plate. In: Carlson DS, Goldstein SA, eds. Bone Biodynamics in Orthodontic and Orthopedic Treatment. Craniofacial Growth Series. Ann Arbor, MI: Center for Human Growth and Development; 1992:93–110.
- Laferriere KA, Castellano RD.Experience with percutaneous suspension of the malar fat pad for midface rejuvenation.Facial Plast Surg Clin North Am. 2005Aug;1333939
- Lazenby RA. 1990. Continuing periosteal apposition. I. Documentation, hypotheses, and interpretation. Am. J. Phys. Anthropol. 82:451–72
- LeeS.IsseN.Barbed polypropylene sutures for mid-face elevation: early results”. Arch. Facial Plast. Surg. 7: 55, 2005
- Lemperle G. alia – Foreign body granulomas after all injectable Dermal fillers: I possible causes. – PRSJ 2008 Lemperle G. alia – Foreign body granulomas after all injectable dermal fillers: part 2. Treatment options. PRSJ 2008
- Lewandowska, I. Staniszewska, M. Baran, M. Turczynowicz, and P. Retman, “Complications After Polydioxanone Threads (PDO) for Facial Lifting – A Literature Review,” Journal of Education, Health and Sport 66 (2024): 50072.
- LewisR. P.SchweitzerJ.OdumB. C.LaraW. C.EdlichR. F.GampperT. J.Sheets, 3-D strands, trimensional (3-D) shapes, and sutures of either reinforced or nonreinforced expanded polytetrafluoroethylene for facial soft-tissue suspension, augmentation, and reconstruction.J Long Term Eff Med Implants 1998811942
- Li J. Et al.: A dual peptide sustained-release system based on nanohydroxyapatite/polyamide 6,6 scaffold for synergistic-enhancing diabetic rats fracture healing in osteogenesis and angiogenesis. Bioingineeriing and Biotechnology. 26 may 2021. 2010
- Li, Z. H. Li, X. Y. Chen, W. S. Xing, and J. T. Hu, “Facial Thread Lifting Complications in China: Analysis and Treatment,” Plastic and Reconstructive Surgery. Global Open 9 (2021): e3820.
- Liu Y, Advancements in adipose-derived stem cell therapy for skin fibrosis. World J Stem Cell. 2023 May 26;15(5):342–353.
- MaasC. S.MerwinG. E.WilsonJ.FreyM. D.MavesM. D.Comparison of biomaterials for facial bone augmentation.Arch Otolaryngol Head Neck Surg 1990May;11655516
- Manag Abdullah. Recent Advancement on Polyamide Composites as an Alloplastic Alternative in 3D Printing for Craniofacial Reconstruction. January 2024. In book: Functional Bio-based Materials for Regenerative Medicine: From Bench to Bedside (Part 2) (pp.1-14)
- Martino F., Perestrelo A.R., Vinarský V., Pagliari S., Forte G. Cellular Mechanotransduction: From Tension to Function. Front. Physiol. 2018;9:824.
- Massari L., Benazzo F., Falez F., Perugia D., Pietrogrande L., Setti S., Osti R., Vaienti E., Ruosi C., Cadossi R. Biophysical stimulation of bone and cartilage: State of the art and future perspectives. Int. Orthop. 2019;43:539–551.
- Mathis M, Pure hydrolysis of polyamides: a comparative study. Polymer Science 18 august 2023.
- Meretsky C., Advances in Tissue Engineering and Its Future in Regenerative Medicine Compared to Traditional Reconstructive Techniques: A Comparative Analysis. Cureus. 2024 Sep 7;16(9):e68872. doi: 10.7759/cureus.68872Cureus. 2024 Sep 7;16(9):e68872.
- Minore A, Intralesional and topical treatments for Peyronie’s disease: a narrative review of current knowledge. Asian J Androl. 2024 Aug 23
- Mitash N: Inhibition of YAP/TAZ signaling by the FDA approved drug verteporfin attenuate fibrosis in mouse and human tissue. Am J Respir Crit Care Med 2022;205:A5226 I
- Mohede D., et al.: Verteporfin as a medical treatment in Peyronie’s disease. Sexual Medicine. 10. 2018
- MoenningJ. E.WolfordL. M. Chin augmentation with various alloplastic materials: a comparative study.Int J Adult Orthodon Orthognath Surg 19894317587
- Mohanty, A.K.; Sustainable Polymers. Nat. Rev. Methods Primers 2022, 2, 1–27.
- Monstrey S., et al.: Updated scar management practical guidelines: non-invasive and invasive measures. J Plastic, Reconstructive Aesthetic Surgery (2014) 67,1017-1025
- Morena F., Argentati C., Calzoni E., Cordellini M., Emiliani C., D′Angelo F., Martino S. Ex-vivo tissues engineering modeling for reconstructive surgery using human adult adipose stem cells and polymeric nanostructured matrix. Nanomaterials. 2016;6:57.
- Moss ML, Salentijn L. The primary role of functional matrices in facial growth. Am J Orthod. 1969;55:566–577.
- Naqvi S. N., Stem Cell Mechanobiology and the Role of Biomaterials in Governing Mechanotransduction and Matrix Production for Tissue Regeneration. . Bioeng. Biotechnol. , 14 December 2020. Sec. Biomaterials.Volume 8 – 2020
- Niu, K. Zhang, W. Yao, et al., “A Meta-Analysis and Systematic Review of the Incidences of Complications Following Facial Thread-Lifting,” Aesthetic Plastic Surgery 45 (2021): 2148–2158.
- OdumB. C.BussardG. M.LewisR. P.LaraW. C.EdlichR. F.GampperT. J.High-density porous polyethylene for facial bone augmentation.J Long Term Eff Med Implants
- Okolie O. Bio-based sustainable polymers and materials: from processing to biodegradation. J. Compos. Sci. 2023, 7(6), 213.
- Park, S.-B. Kim, A. Suwanchinda, and K.-H. Yi, “Non-surgical Rhinoplasty Through Minimal Invasive Nose Thread Procedures: Adverse Effects and Prevention Methods,” Skin Research and Technology 30 (2024): e13590.
- Paul.Complications of barbed sutures.Aesthet Plast Surg, 32 (2008), pp. 149
- Perin D. Development of polyamide 6/polycaprolattone (PCL) thermoplastic self-healing polymer blends for multifunctional structural composites. Applied Science 2022,12,12357 : The aim of this work is to develop a polyamide 6 (PA6) matrix with self-healing properties.
- Pinkhasov AM, Contemporary nonsurgical management of Peyronie’s disease. Curr Opin Urol. 2025 Mar 1;35(2):135-141
- Pompeu M. – Foreign body granuloma treatment with 22-MHz ultrasound-guided corticoid infiltration. Journal of Cosmetic Dermatology. 2018
- Qian Xu. Tissue engineering scaffold material of porous nanohydroxyapatite/polyamide 66. Int J Nanomedicine 2010 May 13;5:331–335
- RachelJ. D.LackE. B.LarsonB.Incidence of complications and early recurrence in 29 patients after facial rejuvenation with barbed suture lifting // Dermatol. Surgery.- 2010348354
- RashidR. M.SartoriM.WhiteL.E et Alii: “Breaking strength of barbed polypropylene sutures: rater-blinded, controlled comparison with non-barbed sutures of various calibersArch. Dermatol. 143869722007
- Ratner B. Biomaterials sScience: an introduction to materials in Medicine . 2020.
- Rayat Pisheh H, et al.: How is mechanobiology involved in bone regenerative medicine? Tissue and Cell. 13 may 2022
- Risbud M. Polyamide 6 composite membranes: properties and in bitro biocompatibility evaluation. J biomaterials Sci Polym Ed 2001, 12(1):125-126
- Rizzo A.: LA CHIRURGIA COSMETICA MORFODINAMICA – I NUOVI PARADIGMI DELLA CHIRURGIA ESTETICA. Independently published, Kindle Direct Publishing, 2020.
- Rizzo A: RINOPLASTICA MORFODINAMICA – Alla ricerca dell’armonia, connubio tra estetica, funzionene benessere. Independently published, Kindle Direct Publishing, 2021.
- Rizzo A.: CHIRURGICA COSMETICA MORFODINAMICA: FONDAMENTI BIOLOGICI E CLINICI. In preparazione.
- Robling A.: Biomechanical and molecular regulation of bone remodeling. Ann Rev Biomed Eng. 2006, 8:455-98
- Rubin C, Judex S, Hadjiargyrou M. 2002. Skeletal adaptation to mechanical stimuli in the absence of formation or resorption of bone. J. Musculoskelet. Neuronal Interact. 2:264–67
- Rullan P.P., et al. The use of intralesional sodium thiosulfate to dissolve facial nodules from calcium hydrossiapatite. Dermatologic Surgery 2019;1
- Sakhiyra J. Intralesional agents in dermatology, pros and cons. J of cutaneous and aesthetic surgery. 14(3):p285-295,jul-sep 2021
- Saleh B, Efficacy and Safety of Verapamil Intralesional Injection in Peyronie’s Disease Using the Kalsi Technique. Clinics in Surgery Research Article Published: 01 Jan, 2024
- Safety and complications of absorbable threads made of poly-L-lactic acid and poly lactide/glycolide: Experience with 148 consecutive patients. J Cosmet Dermatol. 2018;17(6):1189-93. 35.
- SasakiG. H.Komorovska-timekE.BennetD. C.CabrielA.An Objective Comparison of Holding, Slippage and Pull-Out Tensions for Eight Suspension Sutures in the Malar Pads of Frech-Frosen Human Cadavers. Aesthetic Surgery Journal, 2008284387396
- Satchanska G. Natural and synthetic polymers for biomedical and envonmental applications. Poltmers. 2024, 16,1159
- Schriefer JL, Warden SJ, Saxon LK, Robling AG, Turner CH. 2005. Cellular accommodation and the response of bone to mechanical loading. J. Biomech. 38:1838–45
- Schwab L.: Polyamide synthesis by hydrolase. University of Groningen
- Serdev N.: Transcutaneous and transmucosal Serdev sutures for nasal tip refinement, alar base narrowing and other corrections. Intech Open 2016. Chapter 6. Serdev N.: Scarless Aptos versus Serdev suture lifting methods. Int Journal of Cosmetic Sirgery, 2004: vol 4-N 2: 1-10
- Serdev N. SERDEV SUTURE TECHNIQUES– Lower SMAS Face LIFT, Original Papers, Int J Cosm Surg, 2010
- Serdev N. P.Chin augmentation using simple suture. Int J Cosm Surg 2001
- Serdev, Nikolay (2008). “Serdev Techniques in Beautification Rhinoplasty”. International Journal of Cosmetic Surgery. 8 (1): 388–469.
- Serdev Nikolay. Miniinvasive Techniques in Rhinoplasty. In Tech Open– 9 marzo 2016
- Serdev N., 2018. “Total Face Beautification using Serdev Sutures,” JOJ Dermatology & Cosmetics, Juniper Publishers Inc., vol. 1(1), pages 18-22, June.
- Serdev N.: Serdev Suture for Buttock’s Lift – Ambulatory Scarless Procedure.The Open Dermatology Journal • 15 Oct 2012
- Serdev N. Transcutaneous scarless buttock lift via tha Serdev Suture Technique. The pmfa Journal vol2 issue 3, feb/mar2015
- Serdev N. P.Year 1994. Suture Suspensions For Lifting Or Volume Augmentation In Face And Body (English version), presented at the 2nd Annual Meeing of the National Bulgarian Society for Aesthetic Surgery and Aesthetic Medicine, Sofia, 18 March 1994, Int J Aesth Cosm, 2001,1:1, 2561-2568
- Serdev N. P. Brow lifting to the upper temporal line 1.5 cm, Int J Aesth Cosm, 2012
- Serdev N. Chin form correction and augmentation using simple suture. Int J Aesth Cosm Beauty Surg IJACBS 2001
- Serdev N. Scarless Serdev Suture Method In Prominent Ears (Bulgarian), Original Papers, Int J Aesth Cosm 2009
- Serdev, Nikolay: Columella Sliding for Nasal Tip Projection Using Septocolumellar Transmucosal Mattress SuturesNikolay P. Serdev 30 November 2015 Published: 09 March 2016
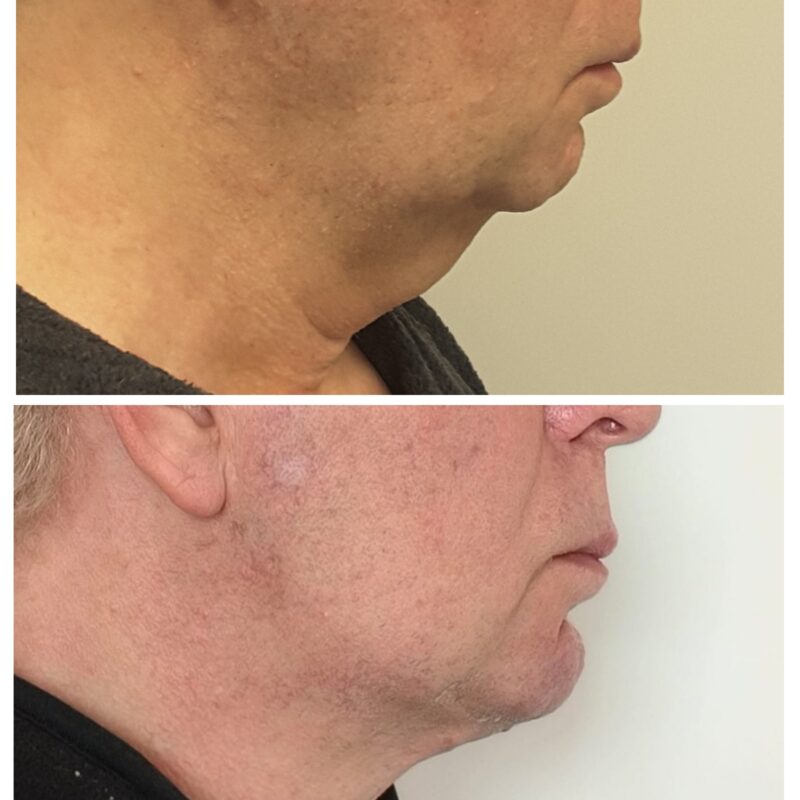
- Serdev Technique for Cervicoal Flaccidity and Mandibular Definition Utilizing “Serdev Sutures”
Written ByRoberto TulliSubmitted: 20 January 2012 Published: 02 October 2013 - Serdev N.Scarless APTOS versus SERDEV suture lifting methods”. Int. Journal of Cosmetic Surgery, 4-N2004
- SerdevN. P.Serdev Suture Techniques Lower SMAS Face Lift, Original Papers, Int J Cosm Surg, 2009
- Serdev, N. (December 2002). “Estiramiento ambulatorio del SMAS en la zona temporal con incisiones mínimas y ocultas”. International Journal of Cosmetic Surgery (in Spanish). 4 (3):1–6
- Shaarawy E, Hegazy RA, Abdel Hay RM. Intralesional botulinum toxin type A equally effective and better tolerated than intralesional steroid in the treatment of keloids: a randomized controlled trial. 2015;14(2):161-6.
- Shakiba M., et al.: Nylon-A material introduction and overview for biomedical applications. Polymers Advanced Technologies. Vol 32, issue 9. September 2021.
- Sheikh Z, et al: Macrophages, foreign body giant cells and their responses to implantable biomaterials. Materials (Basel). 2015 Aug 28;8(9):5671-5701
- SinghS.Baker JL Jr. Use of expanded polytetrafluoroethylene in aesthetic surgery of the face.Clin Plast Surg 2000Oct;27457993
- Smith R., et al.: The enzymatic degradation of polymers in vitro. Wiley Online Library 1987
- Strazzula L, et al.: intralesional sodium thiosulfate for the treatment of calciphylaxis. JAMA Dermatology, 2013; 149(8):946-949
- Su J. Composite scaffolds of mesoporous bioactive glass and polyamide for bone repair. Int J Nanomedicine 2012 May21;7:2547–2555.
- Sulamanidze M.A., I.S. Vozdvizhenskiy, G.M. Sulamanidze, K.M. Sulamanidze and E.G.Experience in Preventive Measures and Treatment of Complications at Face and Neck Thread Rejuvenation Azizyan Published: 02 October 2013
- SulamanidzeM. A.SulamanidzeG. M.SulamanidzeC. M.VozdvizhenskyI. S.Lifting of Soft Tissues With Barbed Threads. Side Effects, Complications. // 11-th ESPRAS Congress Plastic, Restorative and Aesthetic Surgery, 20-26 September 2009Rhodes, Greece.- Book of Abstracts.- 25
- SulamanidzeM. A.SulamanidzeG. M.Aptos Suture Lifting Methods. 10 Years of ExperienceClinics in Plast.Surgery.- 2009April.- 36281306
- Teot L: Textbook on scar management. Springer 2020
- Thadepalli VReview of multifarious applications of polymers in medical and health care textiles Volume 55, Part 2, 2022, Pages 330-336
- Trindade F., et al.: Soybean-modified polyamide-6 mats as a long-term cutaneous woundcovering. Materials Science and Engineering (2019) 957-968.
- Turner CH, Owan I, Takano Y. 1995. Mechanotransduction in bone: role of strain rate. Am. J. Physiol. Endocrinol. Metab. 269:E438–42
- Ullrich M., Biobased polyamides: academic and industrial aspects for their development and applications. Advances in polymer science. Springer, Berlin, Heidelberg, 2022, 1-69.
- Ulrich D., et al.: Human endometrial mesenchymal stem cells modulate the tissue response and mechanical behavior of polyamide mesh implants for pelvic organ prolapse repair. Tissue Engineering. 2014, Part A, Vol 20, N 3-4
- Vining K.H., Mooney D.J. Mechanical forces direct stem cell behaviour in development and regeneration. Nat. Rev. Mol. Cell Biol. 2017;18:728–742.
- Wang PU, Comparing the efficacy and safety of intralesional verapamil with intralesional triamcinolone acetonide in treatmemt of hypertrophic scars and keloids: a meta-analysis of randomized controlled teials. Aesthetic Surgery Journal, vol 41,issue 6, june 2021, pp567-575
- Wang K, “Complications of Thread Lift About Skin Dimpling and Thread Extrusion,” Dermatologic Therapy 33 (2020): e13446.
- Warden SJ, Turner CH. 2004. Mechanotransduction in the cortical bone is most efficient at loading frequencies of 5–10 Hz. Bone 34:261–70
- Warner S., et al.: Botox induced muscle paralysis rapidly degrades bone. Bone 2006 February ; 38(2): 257–264.
- Whaugh D. The efficacy of laser material processing for enhancing stem cell adhesion and growth on different materials (polyamide 6,6). Advances in Contact Angle, Wettability and Adhesion 3 (2018): 373-397.
- Williams D: Biodegradation of surgical polymers. Journal of material science, Material in medicine, 2008.
- M. Winnacker, Polyamides and their functionalization: recent concepts for their applications as biomaterials, Biomater. Sci. 5 (7) (2017) 1230–123
- Winnacker M., et al.: Polyamide/PEG blends as biocompatible biomaterials for the convenient regualation of cell adhesion and growth. Macromolecular Rapid Communications/ Vol 40, 2019.
- Winnacker M., Polyamide derived from terpenes: advances in their synthesis, characterization and applications. European Journal of lipid science and technology. Vol125, issue 5.
- Winnacker M., Terpene-based Polyamide: a sustainable polymer class with huge potenzial. Current opinion in green and sustainable chemistry. Vol 1, june 2023.
- Wollina U. – Nonsurgical facial scar revision by Hyaluronidase. A case series. – Kosmetische Medizin – january 2015 .
- Yao EH., et al.: Applications of ribozyme and pyrrole imidazole Polyamides for cardivascular and renal disease. RNA Technologies in cardiovascular medicine. Springer 2008
- Yi and S. Y. Park, “Volumizing Threads (Jamber) in the Midface and Controlling Side Effects: Clinical Cases,” Archives of Plastic Surgery 51, no. 4 (2024): 350–355.
- Ying L, et al.: Mechanobiology and applications in biomaterials for soft tissue repair and regeneration. Reference Module in Materials Science and Materials Engineering, 31 october 2022
- Yuan M.: Functional Craniology: kinematics and dynamics. Professor of Oral Surgery, Columbia University Dec 4,2003.
- Xiong Y.: Analyzing the behavior of a porous nano-hydroxyapatite/polyamide 66 composite for healing of bone defects. Int J. Nanomed. 9, 485-494. 2014
- Zhang Q, Intralesional injection of adipose-derived stem cells reduces hypertrophic scarring in a rabbit era model.Stem Cell Res Ther. 2015 Aug 18;6(1):145.
- Zhang Y. Stem Cell-Friendly Scaffold Biomaterials: Applications for Bone Tissue Engineering and Regenerative Medicine. journal Frontiers in Bioengineering and Biotechnology. 14 december 2020
- Zhang Y. Mechanical stimulation on mesenchymal stem cells and surrounding microenvironment in bone regeneration: regulations and applications. Cell Dev Biol 21 january 2022.
- Zhou T, Local injection therapy for carpal tunnel syndrome: a network meta-analysis of randomized controlled trial. Front Pharmacolog 24 august 2023. Vol 14 2023.
- Zugail AS, Safety and feasibility of percutaneous needle tunneling with platelet-rich plasma injections for Peyronie’s disease in the outpatient setting: a pilot study. .Int J Impot Res. 2024
Functional Bio-based Materials for Regenerative Medicine: From Bench to Bedside
Mohd Fauzi Mh Busra
Functional Bio-based Materials for Regenerative Medicine: From Bench to Bedside explores the use of bio-based materials for the regeneration of tissues and organs. The book presents an edited collection of 28 topics in 2 parts focused on the translation of these materials from laboratory research (the bench) to practical applications in clinical settings (the bedside). Chapter authors highlight the significance of bio-based materials, such as hydrogels, scaffolds, and nanoparticles, in promoting tissue regeneration and wound healing. Topics included in the book include: – the properties of bio-based materials, including biocompatibility, biodegradability, and the ability to mimic the native extracellular matrix. – fabrication techniques and approaches for functional bio-based material design with desired characteristics like mechanical strength and porosity to promote cellular attachment, proliferation, and differentiation – the incorporation of bioactive molecules, such as growth factors, into bio-based materials to enhance their regenerative potential. – strategies for the controlled release of molecules to create a favorable microenvironment for tissue regeneration. – the challenges and considerations involved in scaling up the production of bio-based materials, ensuring their safety and efficacy, and obtaining regulatory approval for clinical use Part 2 covers advanced materials and techniques used in tissue engineering. Topics focus on advanced composite materials for 3D scaffolds and the repair of tissues in different organs such as the heart, cornea, bone and ligaments. Materials highlighted in this part include polyamide composites, electrospun nanofibers, and different bio-based hydrogels. Functional Bio-based Materials for Regenerative Medicine: From Bench to Bedside is a valuable reference for researchers in biomedical engineering, cell biology, and regenerative medicine who want to update their knowledge on current developments in the synthesis and application of functional biomaterials.
Polyamide derived from terpenes: advances in their synthesis, characterization and applications. Winnacker M.
Polyamides are very important polymers, with applications from commodities up to high-performance materials for, for example, fibers or for the biomedical sector. Nowadays, still most of them are synthesized from fossil resources. With regards to sustainability and bioeconomy, and especially regarding the new structures and properties that can thus be achieved, the preparation of polyamides (PAs) from natural precursors is getting more and more important.
Similar approaches are interesting from a scientific point of view regarding, for example, structure-function-relations, but also with regards to different applications as, for example, high-performance or biomedical materials.
Practical applications: Terpene-based polyamides can find many applications, from commodities up to high-performance fibers and special materials in (bio)medicine, for example, drug delivery, tissue engineering, etc.
Polyamide/PEG Blends as Biocompatible Biomaterials for the Convenient Regulation of Cell Adhesion and Growth
Winnacker M.
In addition to their established usage in textiles, commodities, and automotives, classical polyamides (nylons) are recently becoming increasingly interesting for applications in (bio)medicine. This fact relies on many prosperous properties of these polymers, which are toughness, resistance, biocompatibility, low immunogenicity, tunable biodegradability, and their similarity to natural peptides (amide bonds). Some nylon‐based medical products do already exist for wound treatment applications, implants, and biomolecule‐interacting membranes, but the systematic use of these polymers for tissue engineering is—although desired—still to be accomplished. Inspired by this, the suitability of nylon 6 and of a related biobased and more hydrophobic terpene‐derived polyamide as surfaces for the controlled interaction with HaCat cells (human keratinocytes) are investigated herein with regard to possible applications for regenerative skin replacement. The nylons are applied as neat polymers and as hydrophilized blends/composites with polyethylene glycol and confirm their excellent suitability as biomaterials. Polyamides (nylons), which have been used for textiles, commodities, and automotives for decades, are also becoming increasingly interesting for medical applications. Herein, novel blends consisting of a polyamide (nylon 6 or a biobased, terpene‐based polyamide) and polyethylene glycol (and a corresponding copolymer), as well as their interactions with human keratinocytes, are described. This approach is very promising with regard to skin tissue engineering.
Biobased polyamides: academic and industrial aspects for their development and applications Ullrich M.
Polyamides are very important polymers for a wide range of applications. In the context of Green Chemistry and the development of sustainable polymers from renewable resources, many polyamides have meanwhile been developed that are derived from natural building blocks. In addition to sustainability, biobased polyamides can have special structures and properties that cannot be obtained so easily via fossil-based pathways. This article gives an overview over the recent developments in this field and elucidates the potential of these polymers for different applications.
Transcutaneous scarless buttock lift via tha Serdev Suture Technique
Serdev N
Essential equipment consists of a long, curved, semi-elastic needle and Polycon No 4, 6 or 8 (elastic Bulgarian antimicrobial polycaproamide threads)
Insight into Mechanobiology: How Stem Cells Feel Mechanical Forces and Orchestrate Biological Functions.
Argentati C.
Mechanosensing
All organisms have evolved structures, enabling them to recognize and respond to mechanical forces. This cross-talk takes place at the macroscale level (e.g., in organs and tissues), at the microscale level(e.g., in single cells), and also at the nanoscale level(e.g., inmolecular complexes or single proteins). At present, we know that the different types of forces orchestrate the control of all biological functions, including stem cells’ commitment, determination, development, and maintenance of cells and tissues homeostasis.
Notably, between ECM and stem cells exists a dynamic cross-talk, as stem cells may change the ECM composition and remodel the architecture either by the secretion of ECM structural components and matrix metalloproteinases, or by exerting mechanical forces through the cytoskeleton f ibers. The challenge is to create a suitable cell microenvironment that generates mechanosensing/ mechanotransduction signals and guide stem cells’ functions.
The rationale of the use of biomaterials as stem cells support is based on the cross-talk taking place between them. Stem cells act on biomaterials releasing ECM proteins and bioactive molecules and exert forces through the cytoskeletal components to recreate their niche. Conversely, biomaterials act on stem cells through their intrinsic chemical-physical properties, which activate mechanosensing/mechano- transduction signalling and thereby modulate the stem cells fate. Different types of natural (e.g., collagen, fibrin, silk) and synthetic (e.g., polylactic acid, polyamide, polyesters, polyanhydrides, polyurethane) polymers have been manipulated to fabricate biocompatible films (two-dimensional) or scaffolds (three-dimensional) with tuneable properties to guide stem cells fate.
Mechanical cues activated by the ECM and translated to the cell through mechanosensing/mechano- transduction signals represent a general scheme by which cells, tissues, organs, and whole organisms respond to external mechanical stimuli orchestrating their biologic activity.
Advances in the use of biomaterials as support for in vitro stem cells cultures to generate ex-vivo models of tissues and organs, together with computational systems, have highlighted the potentials of mechanobiology as a new therapeutic tool to be investigated for RM applications.
Tissue engineering scaffold material of porous nanohydroxyapatite/polyamide 66
Qian Xu
Polyamide (PA) has good biocompatibility with human tissue, probably due to its similarity to collagen protein in chemical structure. It has been widely used in the biomaterials application of surgical sutures for
nearly half a century. Especially important, PA also exhibits excellent mechanical properties.
Composite scaffolds of mesoporous bioactive glass and polyamide for bone repair.
Jiacan Su
Polyamide (PA), a polymer with excellent biocompatibility, has been used to fill bone defects and to create porous scaffolds for bone tissue engineering.
Mechanical stimulation on mesenchymal stem cells and surrounding microenvironment in bone regeneration: regulations and applications.
Zhang Y
recent studies proves that external mechanical stimulation regulates bone marrow mesenchymal stem cells (BMSCs) toward osteogenic lineage which is independent of osteocytes regulation (Schreivogel et al., 2019). The bone defect first triggers an inflammatory process, which leads to the recruitment of mesenchymal stem cells (MSCs) to the bone defect by inflammatory factors. These MSCs then differentiate into cartilage that gradually ossifies with the growth of blood vessels into the cartilage model. Thus, MSCs play a crucial role in bone regeneration. MSCs regulate the immuno-microenvironment by interacting with macrophages and regulating blood vessel formation by secreting angiogenic growth factors. This process involves interacting cells, including MSCs, macrophages, and vascular endothelial cells, as well as extracellular matrix molecules and cytokines, all of which constitute the MSC niche that is of great significance in regulating bone regeneration (Moore and Lemischka, 2006; Kuhn and Tuan, 2010; Vafaei et al., 2017).
Previous studies have indicated that MSC differentiation was determined by the MSC niches (Chen et al., 2020). Moreover, recent studies have shown that MSC differentiation was also affected by mechanical stimulation (Ravichandran et al., 2017).
The lacunar-canalicular system (LCS) is filled with interstitial fluid (Timmins and Wall, 1977). Intramedullary pressurization alteration and deformation of bone matrix generate interstitial fluid flow (Kwon et al., 2010; Price et al., 2011; Ciani et al., 2014). Therefore, mechanical loading leads to variation in intramedullary pressurization, which results in shear stress generation. Shear stress applies to osteocytes in LCS and MSCs in the bone marrow. Fluid shear stress is the general form of the force applied to MSCs in the bone marrow under physiological conditions (Gurkan and Akkus, 2008). The form of the force applied to MSCs in the periosteum is mainly caused by micro-deformation of bone generated by external mechanical stimuli such as stretching and compression. MSCs respond to the stimulation indirectly by sensing the micro-deformation of the extracellular matrix. Therefore, when investigating the mechanism of the mechanical loading effect on MSC differentiation, the function of both the direct and indirect force ought to be considered.
A variety of mechanical stimuli can be applied to cells using flexible culture substrates as well as scaffolds or bioreactors with suitable mechanical properties.87, 259 Axial, biaxial and cyclic static stresses have been used to induce cell proliferation.251 Studies have shown that cyclic mechanical strain is determinant in the control of the assembly of cells grown on flexible substrates.260, 261
Stem Cell Mechanobiology and the Role of Biomaterials in Governing Mechanotransduction and Matrix Production for Tissue Regeneration.
Naqvi S.
In conclusion, the future of regenerative medicine is based on (creation of metods) (the fabrication of innovative devices) that take into account the feedback between stem cells biology, cell sensing of force, and biomaterials‟ properties (topography, stiffness, electrical conductibility, in vivo behavior, drugs release and form).
Intralesional Injection Therapy and Atypical Peyronie’s Disease: A Systematic Review.
Choi EJ
Overall, 1,357 patients with PD were treated with intralesional therapy, of which 250 patients were considered to have an atypical presentation. 162 (648%) of the patients were treated with intralesional collagenase Clostridium histolyticum, 49 (19.6%) with verapamil, 29 (11.6%) with interferon alfa-2b, 5 (2.0%) with hyaluronic acid, and another 5 (2.0%) with onabotulinumtoxinA.
Intralesional and topical treatments for Peyronie’s disease: a narrative review of current knowledge.
Minore A
effectiveness and safety profiles of collagenase Clostridium histolyticum (CCH), interferon, platelet-rich plasma (PRP), hyaluronic acid, botulinum toxin, stem cell, extracorporeal shock wave therapy (ESWT), and traction therapy
Intralesional injection of adipose-derived stem cells reduces hypertrophic scarring in a rabbit era model
Zhang Q
Myofibroblast differentiation is another intensifier of fibrosis during wound healing. Myofibroblasts, differentiated from fibroblasts in an injury environment, are intended for narrowing the margin of the wounds and accelerating the re-epithelialization by contraction. However, at the same time, they produce tensed, excessive, and irregularly arranged collagen bundles and bring on over-contraction that characterizes hypertrophic scars [14, 15]. Prolonged wound healing usually results in hypertrophic scarring. Consequently, it is very important to ensure the formation of an adequate microvascular network and development into a permanent vascular network during the healing process; otherwise, wound closure will be impaired and hypertrophic scars will occur [16].
Cells biomodulation: the future of Dermatology.
Antonio CR
The anti-inflammatory action of botulinum toxin in the cutaneous vascularization reduces the inflammatory phase of the cicatricial process; besides, its action in fibroblasts and in the expression of TGF-beta1 acts improving the appearance of the scar.
Pruritus, present in many dermatologic conditions, when peripherally induced (pruriceptive pruritus) shows significant improvement with the application of intradermal botulinum toxin. 19 The molecular mechanisms involved in the improvement of pruritus with botulinum toxin are mast cell stabilization and inhibition of its degradation caused by BonT
in areas affected with hair rarefaction, there is relative hypoxemia, slower capillary filling and high levels of dihydrotestosterone. 27 The enzymatic conversion of testosterone into dihydrotestosterone depends on oxygen. In low concentrations of oxygen, the conversion is favored, leading to increased hair loss, whereas in high concentrations of oxygen, the favored conversion is testosterone into estradiol, favoring reduction of hair loss. Therefore, the application of botulinum toxin in the scalp reduces the vascular pressure when reducing muscular tone, creating increased local vascular flow and, consequently, increased oxygen, which reduces the enzymatic conversion of testosterone into dihydrotestosterone